Hepatitis C Screening and Gender Disparities in Positivity Rates in Argentina: A Multicenter Study
DOI:
https://doi.org/10.52787/agl.v56i1.595Keywords:
Hepatitis C/epidemiology, serologic tests, mass screening, sex factors, mortality, Argentina/epidemiologyAbstract
Introduction. Anti-HCV seropositivity is a public-health concern in Argentina, with potential disparities by gender. We estimated anti-HCV seropositivity in a multicenter public laboratory network, described gender-based differences, and examined the association with all-cause mortality.
Methods. Retrospective observational study with centralized chemiluminescent immunoassay testing at Hospital El Cruce, using samples from 64 public centers from January 1, 2013 to December 31, 2023. The analyses were performed at the patient level (the first test per person), and the positivity rate was calculated for each testing site. Vital status information was obtained from hospital records and RENAPER (with a cut-off date of December 2024). Mortality by anti-HCV serostatus was assessed using logistic regression with a prespecified 2:1 matching on age, gender, and testing site.
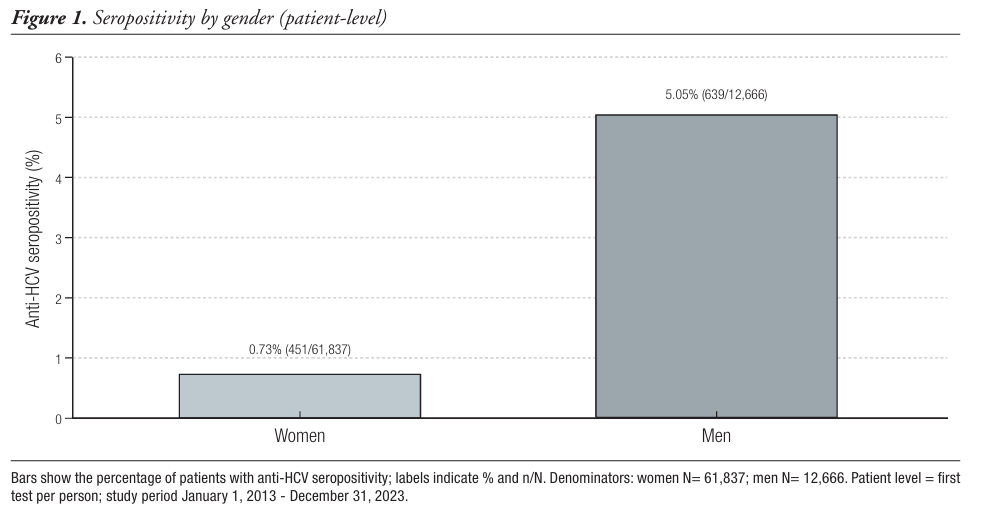
Results. Of the 74,503 adults tested, 1,101 (1.48%) were anti-HCV–positive. Of those tested, 83.0% were women (61,837/74,503) and 17.0% were men (12,666/74,503). Within gender, seropositivity was 0.73% in women (451/61,837) and 5.05% in men (639/12,666). The per-test positivity rate was 0.5% in peripheral centers (451/90,194) and 5.1% in the hospital (922/18,082). Of the individuals who tested positive for anti-HCV, 25.0% (275/1,101) were deceased at the cut-off date. In a matched cohort of 2:1 by age, gender, and site, anti-HCV positivity was associated with a higher risk of death (adjusted OR 4.75; 95% CI 3.82–5.94; p < 0.001).
Conclusions. Men were tested much less frequently than women (17.0% versus 83.0% of those tested), yet they were far more likely to test positive for anti-HCV (5.05% versus 0.73% within gender), accounting for the majority of positive results (58%). Therefore, screening policies should prioritize increasing testing among men, especially in high-yield hospital settings, and ensure rapid linkage to care. The association between anti-HCV seropositivity and higher mortality reinforces the urgency of these actions.
References
-1. World Health Organization. Global health sector strategy on viral hepatitis 2016–2021: towards ending viral hepatitis. Geneva: World Health Organization; 2016.
-2. Averhoff FM, Glass N, Holtzman D. Global burden of hepatitis C: considerations for healthcare providers in the United States. Clin Infect Dis. 2012;55(Suppl 1):S10–S15. doi:10.1093/cid/cis361.
-3. Kretzer IF, Livramento A do, Cunha J da, Gonçalves SN, Tosin I, Spada C, et al. Hepatitis C worldwide and in Brazil: silent epidemic—data on disease including incidence, transmission, prevention, and treatment. ScientificWorldJournal. 2014;2014:827849. doi:10.1155/2014/827849.
-4. Petruzziello A, Marigliano S, Loquercio G, Cozzolino A, Cacciapuoti C. Global epidemiology of hepatitis C virus infection: an update of the distribution and circulation of hepatitis C virus genotypes. World J Gastroenterol. 2016;22(34):7824-7840. doi:10.3748/wjg.v22.i34.7824.
-5. Gaite LA, Marciano S, Galdame OA, Gadano AC. Hepatitis C in Argentina: epidemiology and treatment. Hepat Med. 2014;6:35-43.
-6. Alessandrini R, Calfunao D, Perez R, Torresin J, Bouza MF. Point-of-care testing for HCV and HBV infection: first experience in Patagonia, Argentina. Int J Infect Dis. 2018;73(Suppl 1):206. doi:10.1016/j.ijid.2018.04.3881.
-7. McCombs JS, Matsuda T, Tonnu-Mihara I, Saab S, Hines P, L’Italien G, et al. The risk of long-term morbidity and mortality in patients with chronic hepatitis C. JAMA Intern Med. 2014;174(2):204-212. doi:10.1001/jamainternmed.2013.12505.
-8. Neal KR. Excess mortality rates in a cohort of patients infected with the hepatitis C virus: a prospective study. Gut. 2007;56(8):1098-1104. doi:10.1136/gut.2006.113217.
-9. Omland LH, Jepsen P, Krarup H, Schønning K, Lind B, Kromann-Andersen H, et al. Increased mortality among persons infected with hepatitis C virus. Clin Gastroenterol Hepatol. 2011;9(1):71-78. doi:10.1016/j.cgh.2010.09.014.
-10. Vaidya V, Partha G, Karmakar M. Gender differences in utilization of preventive care services in the United States. J Womens Health (Larchmt). 2012;21(2):140-145. doi:10.1089/jwh.2011.2876.
-11. Mendizabal M, et al. Prevalence of hepatitis C in Buenos Aires Province: a population-based study. J Viral Hepat. 2020;27(12):1320-1327. doi:10.1111/jvh.13363.
-12. Cobos M, Hidalgo G, Soratti C. Serologic profile of donors in Argentina. Transplant Proc. 2023;55(6):1473-1476. doi:10.1016/j.transproceed.2023.03.076.
-13. Flichman D, Blejer JL, Livellara BI, Ré V, Bartoli S, Bustos JA, et al. Prevalence and trends of markers of hepatitis B, C, and HIV in Argentine blood donors. BMC Infect Dis. 2014;14:218. doi:10.1186/1471-2334-14-218.
-14. Lacey C, Ellen S, Devlin H, Wright E, Mijch A. Hepatitis C in psychiatry inpatients: testing rates, prevalence and risk behaviours. Australas Psychiatry. 2007;15(4):315-319. doi:10.1080/10398560701358113.
-15. Adaszko D, et al. Epidemiología de la hepatitis C en Argentina: revisión sistemática. Buenos Aires: Ministerio de Salud de la Nación; 2017.
-16. Cobo B, Cruz CT, Dick P. Gender and racial inequalities in the access to and the use of Brazilian health services [dataset]. Figshare. 2022. doi:10.6084/m9.figshare.19922366.
-17. Lin CF, Shiau TJ, Ko YC, Chen PH, Wang JD. Prevalence and determinants of biochemical dysfunction of the liver in Atayal aboriginal community of Taiwan: is betel nut chewing a risk factor? BMC Gastroenterol. 2008;8:13. doi:10.1186/1471-230X-8-13.
-18. El-Kamary SS, Jhaveri R, Shardell M. All-cause, liver-related, and non–liver-related mortality among HCV-infected individuals in the general US population. Clin Infect Dis. 2011;53(2):150-157. doi:10.1093/cid/cir306.
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Manuel Barbero, Ignacio Roca, Lucía Navarro, Nicolás Domínguez, Omar Galdame, María Del Carmen Puente, Laura González, Lucía Guillén, María Virginia Gustincic, Fernando Cairo

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.












